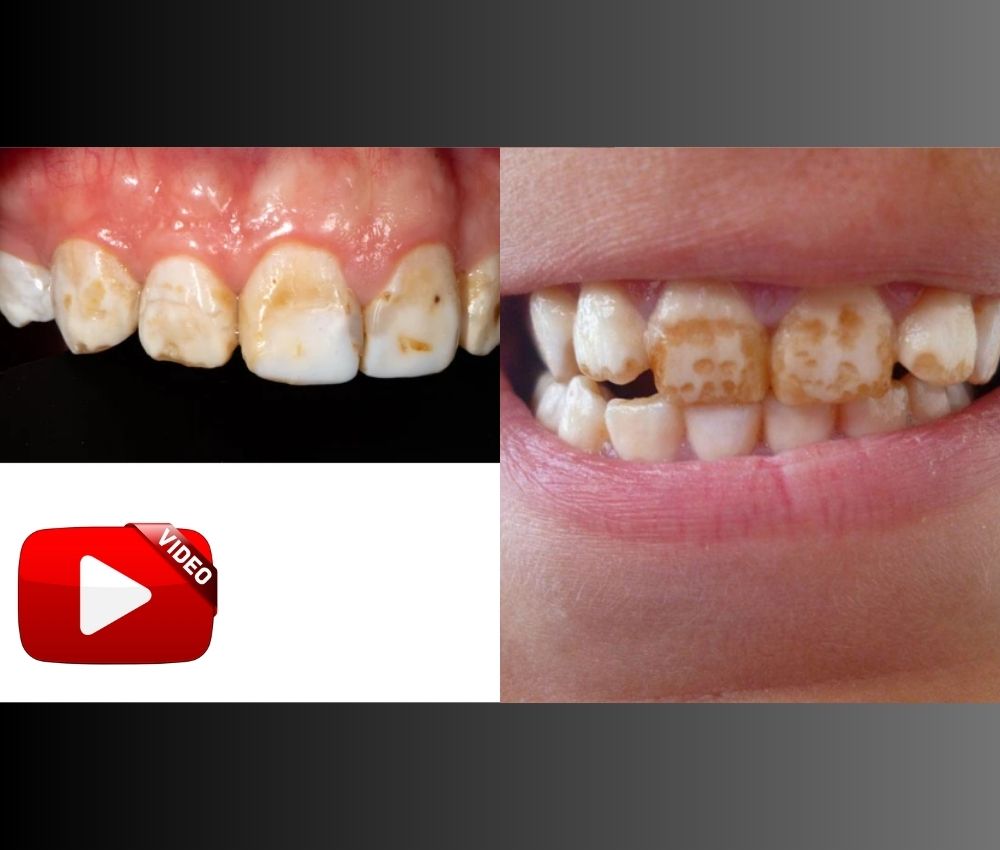
Fluoride toxicity in children remains a significant clinical concern due to the widespread use of fluoride-containing products in pediatric oral health. While fluoride is essential for dental caries prevention, excessive ingestion can lead to acute or chronic toxicity, compromising systemic health.
📌 Recommended Article :
Dental Article 🔽 Fluoride in Pediatric Dentistry: Dosage, Frequency, and Current Controversies ... Key aspects include topical vs. systemic fluoride, caries-preventive effectiveness, and a special update on recent FDA considerations (2025) related to systemic fluoride supplements.This article provides an updated, evidence-based, and SEO-optimized review of symptoms, emergency actions, preventive strategies, and comprehensive management of fluoride toxicity in the pediatric population.
Advertisement
✅ Overview of Fluoride Toxicity
Fluoride toxicity occurs when the ingested dose exceeds the body’s capacity to metabolize and excrete fluoride safely. The probable toxic dose (PTD) is approximately 5 mg/kg body weight, and ingestion above this threshold requires emergency assessment (AAPD, 2023).
Excessive exposure can arise from toothpaste, mouth rinses, dietary supplements, or accidental ingestion of professional topical fluoride products.
📌 Recommended Article :
Dental Article 🔽 Silver Diamine Fluoride in Pediatric Dentistry: A Review ... Silver Diamine Fluoride (SDF) has emerged as a non-invasive and cost-effective treatment for managing dental caries in children.✅ How Fluoride Toxicity Affects General Health
➤ Systemic Impact
Excessive fluoride affects multiple body systems:
▪️ Gastrointestinal system: irritation of gastric mucosa causing nausea, vomiting, abdominal pain.
▪️ Electrolyte balance: risk of hypocalcemia and hyperkalemia due to fluoride’s strong affinity for calcium ions.
▪️ Neuromuscular system: muscle spasms, paresthesia, and in severe cases, seizures.
▪️ Cardiovascular system: altered cardiac function from electrolyte imbalance.
▪️ Skeletal development: chronic high intake may result in dental fluorosis and skeletal fluorosis.
📌 Recommended Article :
Dental Article 🔽 Fluoride Varnish in Pediatric Dentistry: Benefits, Indications, Mechanism, and Application Protocol ... Due to its ease of application, safety, and efficacy, it has become an essential part of caries management in clinical pediatric practice.✅ Early Signs and Symptoms of Fluoride Toxicity in Children
➤ Mild to moderate ingestion may present with:
▪️ Nausea and vomiting (often the earliest sign)
▪️ Hypersalivation
▪️ Abdominal pain
▪️ Diarrhea
▪️ Headache
▪️ Weakness or fatigue
➤ Severe ingestion may lead to:
▪️ Hypocalcemia-related tetany
▪️ Cardiac arrhythmias
▪️ Seizures
▪️ Respiratory depression
▪️ Life-threatening toxicity if untreated
Children are at higher risk because of lower body weight and tendency to swallow toothpaste.
📌 Recommended Article :
Dental Article 🔽 Enamel Hypoplasia vs Dental Fluorosis: Key Differences, Diagnosis, and Treatment ... Enamel hypoplasia and dental fluorosis are two developmental defects of enamel frequently encountered in clinical dentistry.✅ Immediate Actions When Fluoride Toxicity Is Suspected
➤ Emergency Management Protocol
1. Assess the amount ingested and body weight to estimate toxicity risk.
2. Administer milk or calcium-rich products immediately to bind fluoride and reduce absorption.
3. Do NOT induce vomiting.
4. Seek emergency medical evaluation, especially if ingestion approaches or exceeds 5 mg/kg.
5. Monitor vital signs and prepare for electrolyte correction in a clinical setting.
6. Severe cases may require IV calcium gluconate, cardiac monitoring, and supportive therapy.
📌 Recommended Article :
Webinar 🔽 Webinar: Silver Diamine Fluoride – A Silver Renaissance in Dentistry - Dr. Anas Al Salami ... Silver Diamine Fluoride (SDF) has emerged as a transformative option in pediatric dentistry, marking a true renaissance in caries management.✅ Prevention Strategies in Pediatric Dental Care
➤ Evidence-Based Prevention Measures
▪️ Parents should supervise brushing until at least age 6.
▪️ Use smear layer of toothpaste for children under 3; use a pea-sized amount from ages 3–6 (CDC, 2024).
▪️ Store fluoride products out of children’s reach.
▪️ Avoid flavored toothpaste that encourages swallowing.
▪️ Evaluate dietary fluoride sources: water fluoridation, supplements, combined exposures.
▪️ Provide structured parental counseling during dental visits.
📊 Comparative Table: Fluoride Sources in Children
| Aspect | Advantages | Limitations |
|---|---|---|
| Community Water Fluoridation | Reduces caries at population level | Risk of overexposure if combined with supplements |
| Fluoride Toothpaste | Highly effective; easy to access | Children may swallow excessive amounts if unsupervised |
💬 Discussion
The balance between the preventive benefits of fluoride and the risks of toxicity requires strategic dosing, parental education, and clinician guidance. Most toxicity events are preventable and relate to unsupervised access or incorrect use of fluoride-containing products. Updated protocols from ADA and CDC emphasize minimizing risk through tailored dosing and behavioral supervision.
📌 Recommended Article :
PDF 🔽 Fluoride Varnish in the Prevention of Dental Caries in Children and Adolescents: A Systematic Review ... We share an article that reviews the literature and develops a protocol for the use of fluoride varnish as a caries preventive agent in children and adolescents.✍️ Conclusion
Fluoride toxicity in children is rare but potentially serious. Early recognition of symptoms, prompt emergency actions, and preventive strategies are crucial to ensuring safety. When used correctly, fluoride remains one of the most powerful tools for caries prevention in pediatric dentistry. Clinicians must continue reinforcing safe use to eliminate avoidable toxic exposures.
🔎 Recommendations
▪️ Educate parents on appropriate fluoride dosing based on age.
▪️ Emphasize supervision during brushing.
▪️ Assess total fluoride exposure at every dental visit.
▪️ Maintain updated emergency protocols for accidental ingestion.
▪️ Promote community awareness regarding the safe storage of dental products.
📚 References
✔ American Academy of Pediatric Dentistry. (2023). Policy on use of fluoride. AAPD Reference Manual. https://www.aapd.org
✔ Centers for Disease Control and Prevention. (2024). Children’s oral health: Fluoride use. U.S. Department of Health and Human Services. https://www.cdc.gov
✔ Agency for Toxic Substances and Disease Registry. (2023). Toxicological profile for fluoride. U.S. Department of Health and Human Services. https://www.atsdr.cdc.gov
✔ Whitford, G. M. (2011). Fluoride in dental products: Safety considerations. Journal of Dental Research, 90(6), 573–582. https://doi.org/10.1177/0022034510384626
📌 More Recommended Items
► Latest FDA Guidelines (2025) on Fluoride Use in Children: What Dentists Need to Know
► Xylitol and Dental Caries Prevention in Children: Mechanism, Benefits, and Clinical Use
► Fluoride Recommendations for Children in the US: What Parents Should Know